Blogs
With over 40 years of experience, we have a proven track record of providing best in class, proprietary products that meet the specific needs of ophthalmologists. Have a look!
CE Mark for Artiplus Toric and Precizon Go Toric marks a new chapter in Ophtec’s portfolio
Groningen, Netherlands, August 2025 – Ophtec announces CE Mark approval for two toric intraocular...
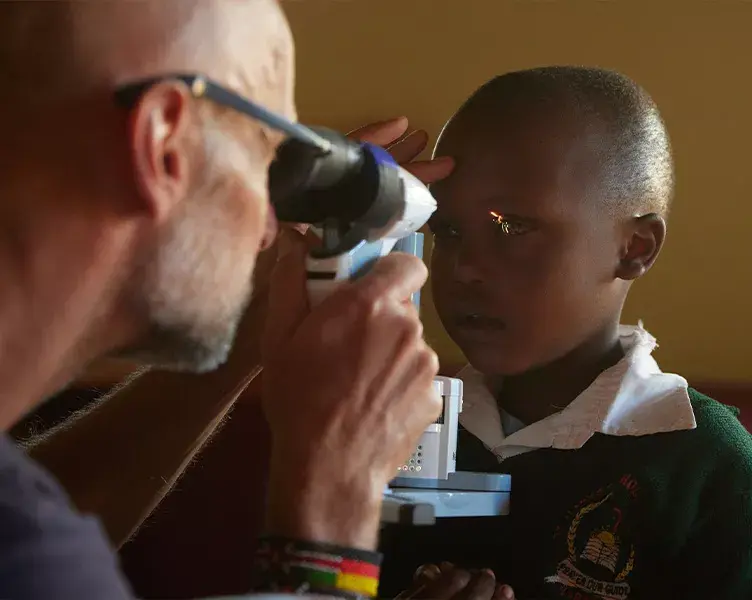
Read moreOphtec Germany supports a relief project with Artisan Aphakia lenses
Ophtec regularly engages in relief projects by supporting ophthalmic surgeons during humanitarian...
Read morePrecizon Go: from an optometrist's perspective
Nicole Stein, a freelance optometrist from Berlin, is a firm believer in the new Precizon Go IOL....
Read moreProduct development at Ophtec is an ongoing process
“As a company, you simply have to keep developing to have a future. Especially where your own speciality is concerned.” Development Leader Paolo Soleri enjoys working on new products, particularly if Ophtec can set itself apart with these products. “Other market parties produce lenses that are placed behind the iris; we make lenses that are placed in front of the iris. Our ‘iris-fixated lens’ concept is one of our key products. Even after 35 years it still offers original solutions for the replacement of glasses and cataract surgery.”
Read moreRecap ESCRS 2024 Barcelona
The ESCRS 2024 took place from September 6-10 in the Fira Barcelona Gran Via, in Barcelona. Ophtec...
Read moreCharity Run – we run together in aid of the Hakuna Matata Foundation
At Ophtec we have known Dr. Christof Knebel for several years. Together with his wife Ute Simon, he...
Read moreFive Frequently Asked Questions About Ringject and CTR
In the field of ophthalmology, Capsular Tension Rings (CTRs) are indispensable tools, tackling...
Read moreTechnology Highlight: CTF Technology
How does Precizon Presbyopic CTF achieve a smooth transition from near to distance, including all...
Read moreNew Developments: Precizon Presbyopic Toric IOL
After the successful introduction of the Precizon Toric, six years ago, and the Precizon...
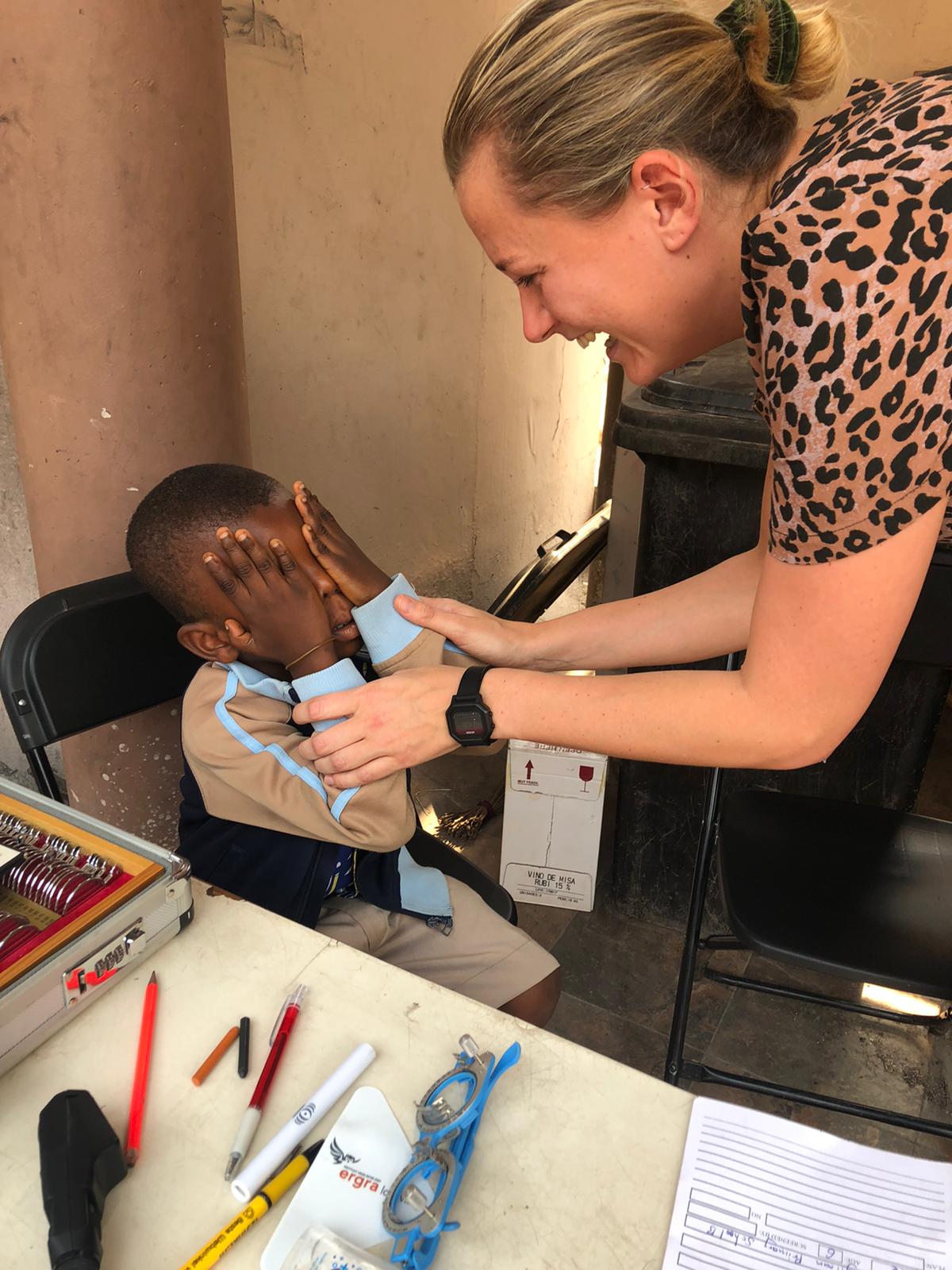
Read moreIris de Jong, eye care volunteer in Ghana
Ophtec’s Account Manager, Iris de Jong has worked as an eyecare volunteer in remote areas of Ghana...
Read moreArtiflex, the best of two worlds
Many different IOLs and PIOLs have been developed and marketed since Harold Ridley's famous first...
Read more